Empowering practices to transform mental health
Change the way you work with patients using tools that promote collaboration to enrich every interaction, in and out of session.

Collaborate together
A fully integrated suite of mental health practice management products
We make it simple to build and manage a flexible practice to ensure you are always providing the highest quality of care.
Speakbox products power modern clinical practices from intake to discharge with support for in person and virtual sessions, elegant session notes, and everything in between.
Speakbox also helps patients manage their wellness between sessions and report on their progress, while maintaining visibility with their care team to maximize the care they receive.
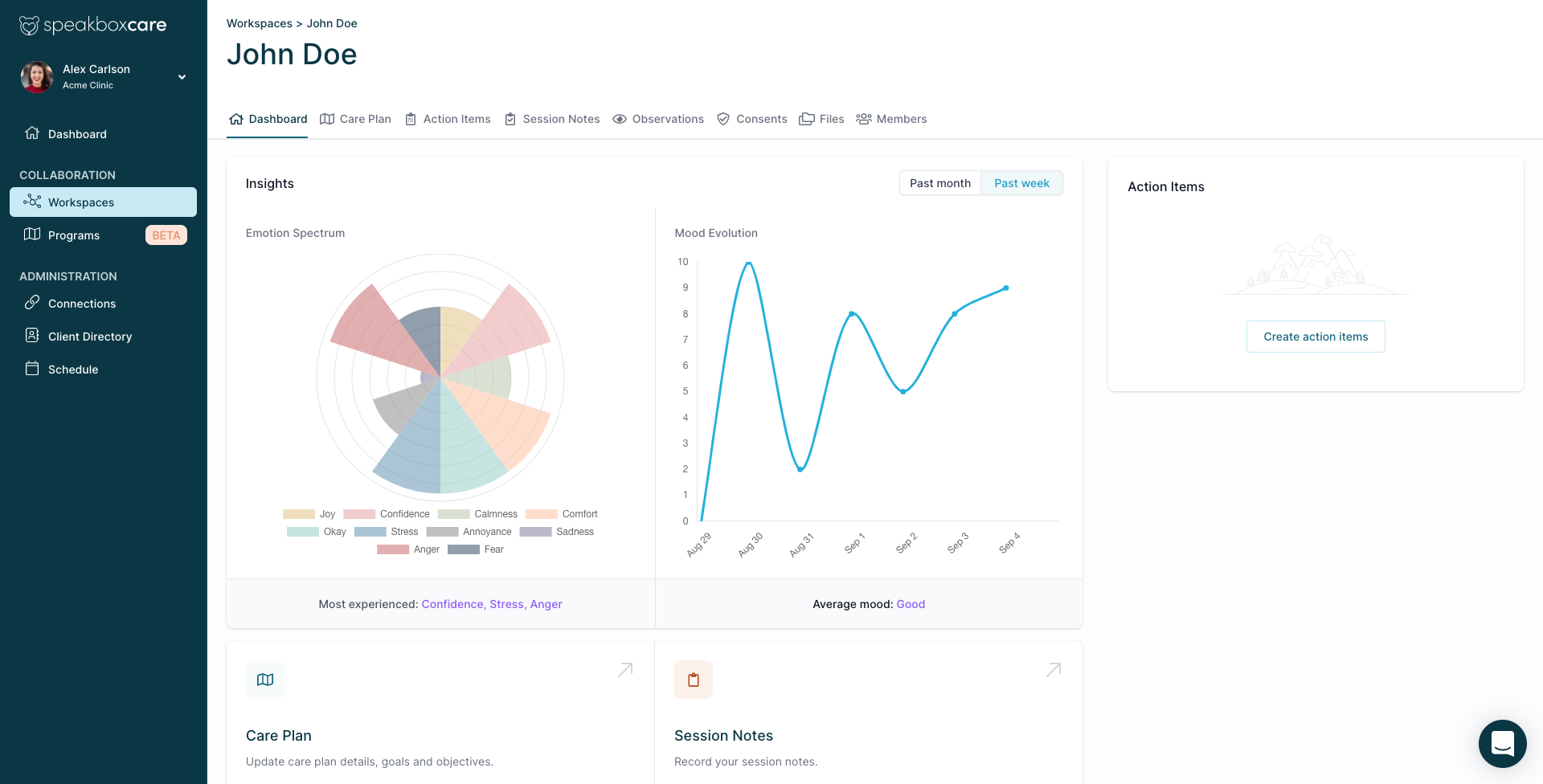
Collaborative Care Platform
From maintaining health records to full-service practice management, Speakbox provides a secure and compliant platform, built to grow with your practice, keeping clients at the center of their care.
-
HIPAA & PIPEDA compliant
-
Share session notes
-
Simple consent & document management
-
Scheduling and video conferencing
-
Support available in real-time


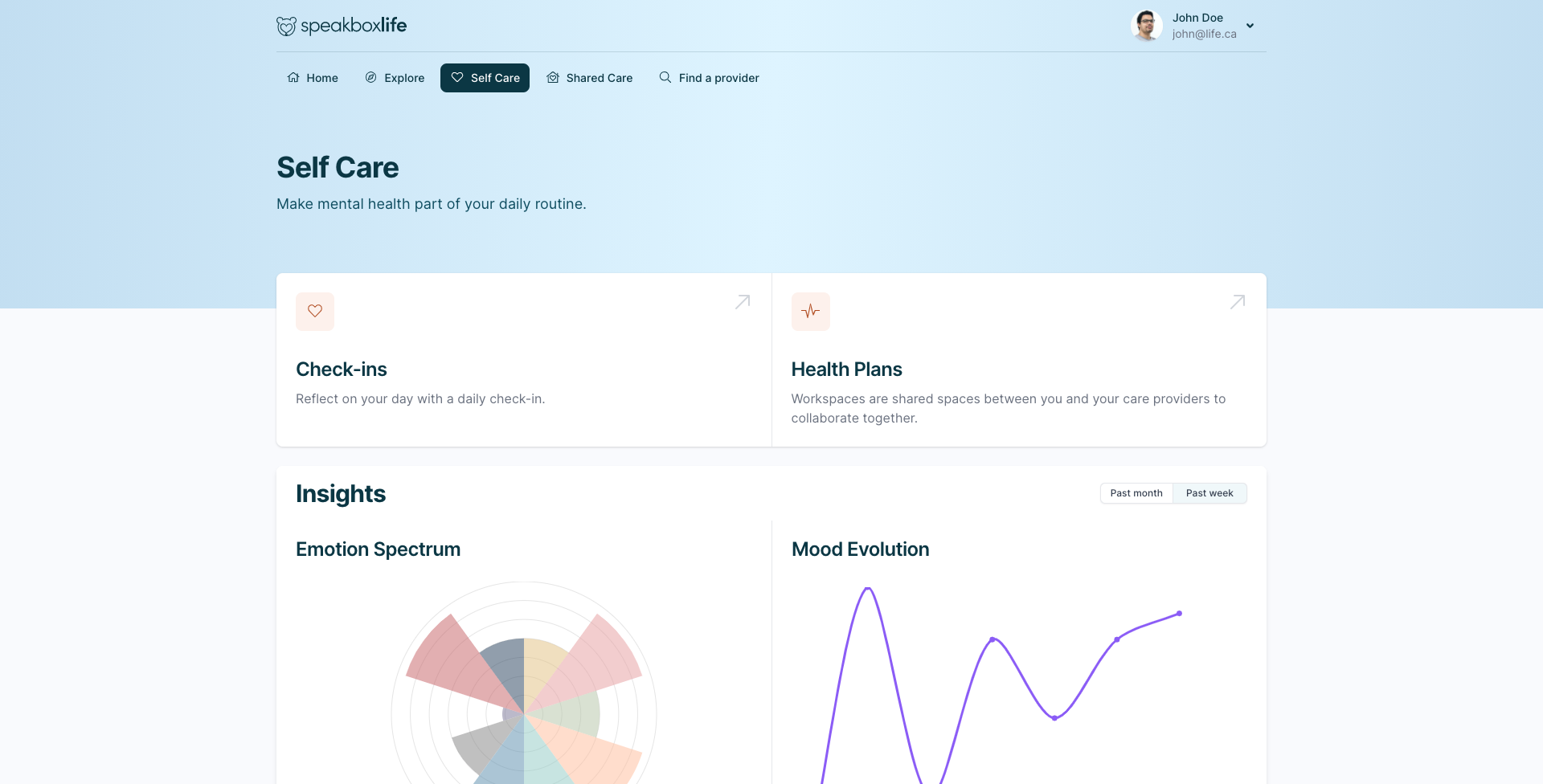
Integrated Patient Platform
We make self-care easy for patients with an intuitive platform and easy to use app.
Whether you collaborate with a care team or want to start investing in your mental health, we made self-care easy, just for you.
-
Desktop and mobile-friendly tools for simple self-care
-
Connect with clinicians who invest in you
-
Seamless video sessions with professionals across North America
-
Access resources and activities to support your mental health

I feel so secure in knowing that I can share my notes and documents with my clients online on an encrypted, Canadian platform. Thank you Speakbox for fewer paper files & emails and more security & collaboration.

Mental health in numbers
We are making a difference
Mental health care is near and dear to everyone at Speakbox.
We aspire to change the relationship
our communities have with mental health, and empower clinicians to do the work they love.
Take a look at the impact we’re having.
280+ hours Estimated hours professionals save each year on administration and paperwork.
72% Clinicians report greater engagement from patients generating more value from each session.
80% Individuals report reduced feelings of stigma having a space to record emotions and access resources.
Our mantra
#healthunobstructed
We believe in people being at the centre of their mental health care.
Let's create a community that celebrates a culture of positive health outcomes.